







It has been referred to as “moobs”, “man-boobs”, “man breasts”, and other fairly demeaning terms since it was first described. In reality, all males are born with breast tissue, and during puberty, the male breast is exposed to a milieu of hormones. During this exposure period, over 70% of adolescents undergo breast development. This is normal during puberty, and three out of four boys will resolve this breast enlargement without intervention. In the 25% that do not resolve, the gland itself is larger than 4 centimeters in 90% of cases.
These patients are commonly followed throughout puberty, and when puberty is largely over, they can be treated either medically or surgically via gynecomastia surgery.

In patients that have gynecomastia after puberty, the breast remains developed, and can be graded into four separate grades:
Lastly, there is a grade of gynecomastia known as “pseudogynecomastia”. Pseudogynecomastia refers to the accumulation of fat in the breast due to obesity. This presentation does not have a definable breast capsule on examination. These patients commonly present with what appears to be grade III or IV gynecomastia, but in reality, their glandular shape and size is being defined more by overall body weight rather than testosterone/estrogen balance.
Treatment for these individuals start with medically supervised weight loss, and then re-evaluating them after weight loss to see if they require further plastic surgery intervention to achieve the desired look.
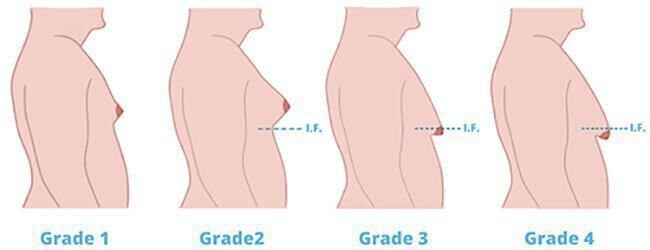
In patients that have gynecomastia after puberty, the breast remains developed, and can be graded into 4 separate grades. Dr. Durkin is a Board Certified Plastic Surgeon in Vero Beach, FL.
There are a number of causes of gynecomastia, but the root cause (pathophysiology) of gynecomastia is an elevated level of estrogen as compared to androgens (specifically testosterone and its cousins) in men.
This is why gynecomastia commonly manifests itself during puberty, as that is the first stage in life where testosterone levels markedly increase. This increased level of testosterone leads to increased levels of estrogens in the body due to the effects of a specific enzyme known as “aromatase”. Aromatase converts testosterone into estrogens, which can then exert a “feminizing” effect on the male breast which we call gynecomastia. This is the root cause of man-boobs. There are a number of stimulants to gynecomastia that increase the effect of this process. Specific causes of gynecomastia include:
These ten listed medications and disease states ALL increase systemic estrogens, or increase the rate of conversion of testosterone to estrogen. The end result of this is development or maintenance of gynecomastia. There are many other medications and disease states that cause gynecomastia. A comprehensive list of medicinal causes can be found on medscape.
Medical treatment is geared towards reducing free estrogen/estradiol within the body system. In the context of non-bodybuilders, medical therapy can be very effective, as it reduces the internal conversion of physiologic testosterone to estradiol.
Further therapy is designed to reduce the conversion of androgens into estrogens. These include aromatase inhibitors such as anastrozole. Other therapies act to block estrogen receptor binding, such as Tamoxifen, but this approach is associated with greater side effects. Clomid, or clomiphene, can also be used to treat gynecomastia. This centrally-acting medication reduces the downstream release of estrogen by reducing the negative feedback loop of estrogens on the hypothalamus. This leads to an increased release of Gonadotropin Releasing Hormone (GnRH), leading to increased testosterone release without increased estrogen production.
This medication will reduce breast size in almost half of patients who take it, but only one patient in five will have resolution of their symptoms. Medical treatment for gynecomastia also includes weight control. The aromatase enzyme is found in active fat cells in the body. Patients with significant obesity will often have increased activity levels of aromatase as compared to non-obese patients. As such, obtaining and maintaining an appropriate body weight is a good way to minimize the effects of gynecomastia.
Treatment is generally undertaken using power assist liposuction. This specific type of liposuction employs an oscillating cannula that vibrates at a high rate of speed (4,000 cycles per second to be exact). This vibration allows us to remove a poorly matured capsule without making a formal skin incision on the breast mound. Instead, a small 2mm poke incision is made lateral to the breast, and the entire procedure is done through a poke-hole that is about the size of a skin freckle. There is mild to moderate bruising with this procedure that lasts about 3-7 days, but the recovery time to feeling normal is about 1-2 days. Patients may shower the day after surgery.
This procedure can be done awake, or with a twilight level of anesthesia. We recommend a twilight level of anesthesia for the greatest degree of comfort, but will readily provide this procedure with local anesthesia only. Scarring with this procedure is absolutely minimal. Vero Beach Gynecomastia Surgery patients may resume normal activity and exercise five days after the procedure. Ocean Drive Plastic Surgery is the only plastic surgery practice on the Treasure Coast to use this specific technology for breast and body contouring.
Treatment for grade II is commonly based on power-assist liposuction only, but in patients with a more developed breast capsule, a small incision around the areola is commonly required. No skin is removed at this stage of presentation, and scarring is limited to a small 2.5cm incision around the nipple-areolar complex. There is mild to moderate bruising with this procedure that lasts about 3-7 days, but the recovery time to feeling normal is about 1-2 days. Patients may shower the day after surgery. This procedure can be done awake, or with a twilight level of anesthesia. We recommend a twilight level of anesthesia for the greatest degree of comfort, but will readily provide this procedure with local anesthesia only. Patients may resume normal activity and exercise five days after the procedure.
At grade III, the mainstay of treatment becomes open excisional therapy, and liposuction begins to play an accessory role. These patients commonly present with a well developed gland with excess skin in place. As such, three types of incisions can be employed depending upon the presenting anatomy. One incision involves circumferential excision of excess skin around the nipple-areolar complex, and folding the incision into the border between the areola and the chest skin. This is ideal method for treating this disorder, as it allows us to minimize noticeable scarring while simultaneously reducing the amount of excess skin present on the chest wall. In patients with severe excess skin, a “lollipop” incision can be used to reduce the degree of excess skin more effectively, but this type of incision is visible. Most patients try to avoid incisions outside of the nipple-areolar complex as they can be very noticeable when exposed.
The last type of incision is made at the level of the inframammary fold, and involves using a free nipple graft. This type of approach is only used in patients with grade IV gynecomastia, and is often seen in patients who have undergone massive weight loss.
In a word, no it does not. Most customer service representatives will tell you that it is before surgery. However, after the procedure, they will not pay for the surgery even after the appropriate procedure codes are submitted by your plastic surgeon. The insurance carrier will label your procedure as “cosmetic”, and refuse to pay it out. This will then lead the physician, the facility, and the anesthesia provider that worked upon you, to submit separate bills to you. This bill is invariably larger than what you would have paid out of pocket without the insurance carrier’s involvement.
Breast surgery in males is covered by insurance in the presence of a biopsy proven breast cancer. In the absence of a breast cancer, however, insurance carriers define gynecomastia surgery as cosmetic, and decline payment.
Patients should wait for any excisional type of surgery until after puberty. As the majority of cases resolve spontaneously, using any modality more advanced than liposuction prior to the end of puberty is not indicated. Our preferred time to intervene for gynecomastia is between the ages of 18 and 22.
None that are effective in the long term. There are a number of supplements that will reduce edema/swelling in the breast tissue, but they do not create a long-term effect on the breast tissue.
The procedure for gynecomastia only takes 1-2 hours total. Recovery time is quick, usually on the order of 1-3 days. It is not a painful procedure, as it can be done without anything other than local anesthesia. Most patients state that they feel sore for a few days, but complaints of severe pain are very uncommon.
We do not require the use of surgical drains for these procedures.
At Ocean Drive Plastic Surgery, we commonly treat this condition, and because of this, we are able to streamline and reduce our pricing to reflect the volume that we do at our private, beach side surgery center. Please note that we STRONGLY recommend that all procedures be undertaken with anesthesia support. By using anesthesia, patients feel less anxiety during the procedure, which in turn leads to reduced swelling and bruising post-operatively. It is very obvious to Dr. Durkin that patients who receive twilight anesthesia recover quicker than those who elect to proceed with surgery awake. By allowing our anesthesiology team to modulate your pain and your physiologic response during surgery, we can minimize tissue trauma, and provide a more comfortable and quicker recovery following your procedure. During gynecomastia surgery Vero Beach patients who want a combination of glandular removal and liposuction, Dr. Durkin does require that those patients receive a twilight level of anesthesia. Without some level of systemic anesthesia, patients are too uncomfortable during the procedure, making that approach less than safe.
Luckily, our complication rate for this procedure is less than 1%. The most common complication seen with this surgery is superficial skin infection. As the male breast gland is a contaminated organ, superficial skin infections can occur after this procedure. Treatment usually requires oral antibiotics for 5-7 days. Re-operation after these procedures is incredibly uncommon. Having treated gynecomastia for over ten years, Dr. Durkin can proudly say that he has never had to re-operate on a patient for an infection or a complication from gynecomastia surgery.

A neck lift and strong jawline can restore your appearance and convey youth and energy.
Learn More

Defined facial features and stron jawlines make men appear more youthful.
Learn More
Interested in non-surgical options for your body concerns? Visit Ocean Drive MedSpa for non-surgical alternatives that can help you achieve the body and skin you've always wanted. Our expert team is trained in the latest techniques and technologies to provide you with the best possible results. Say goodbye to expensive and invasive surgeries, and hello to a fresh, new you. Visit our website to learn more and schedule a consultation today.
Visit Ocean Drive MedSpa

At Ocean Drive Plastic Surgery in Vero Beach, Dr. Alan Durkin and their team of providers deliver incredible results tailored to your needs in a relaxing and uplifting atmosphere. Learn more about the Ocean Drive difference by scheduling your one-on-one diagnostic consultation with Dr. Durkin today.